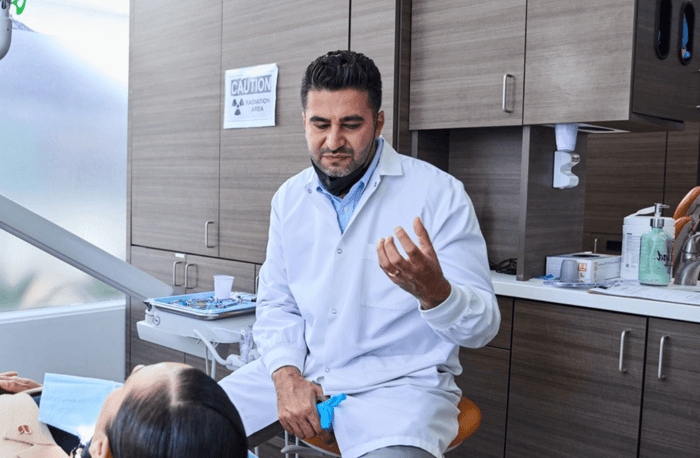
When a toothache lingers longer than it should — or keeps coming back — it's worth taking seriously. Pain that persists, sensitivity that won't quit, and swelling that returns in the same spot are your tooth's way of asking for help.
At See Me Smile Dental & Orthodontics, we offer comprehensive endodontic care in Santa Barbara alongside a full range of dental services, so you never have to chase down a specialist on your own. We use advanced diagnostic tools to catch problems early, when treatment is simpler, and recovery is faster.
This guide walks you through the early indicators you may need an endodontist evaluation, the risk factors worth knowing, and exactly what to expect when you come in. The more you understand, the easier it is to act before a small problem becomes a bigger one.
What Is an Endodontic Evaluation and Why Does It Matter?
An endodontic evaluation is a focused assessment of your tooth's inner health. Your dentist reviews your symptoms, examines the tooth up close, and runs diagnostic tests to determine whether you need specialized care.
What Is an Endodontist?
An endodontist is a dentist who has completed two to three additional years of training after dental school, focusing exclusively on the pulp and root canal system. While your general dentist handles most dental needs, complex or deep-seated infections often call for this level of specialization.
Endodontists work with microscopes and advanced imaging equipment to see what's happening inside your tooth in precise detail. That training and technology give you the best possible chance of keeping your natural tooth.
Common Endodontic Procedures
Root canal treatment is the procedure most people associate with endodontics. It removes infected or damaged pulp, then cleans and seals the space to prevent reinfection. Other procedures include:
Apicoectomy: Surgical removal of the root tip when infection persists after a root canal.
Retreatment: Redoing a previous root canal that didn't heal correctly.
Vital pulp therapy: Treating partially damaged pulp to preserve as much healthy tissue as possible.
Traumatic injury treatment: Addressing teeth damaged in accidents or sports.
Each of these is designed with the same goal: to save your tooth.
Why Early Assessment Matters
Catching a problem early almost always means simpler, less costly treatment. A tooth identified at the right stage may need only a standard root canal. Left untreated, the same tooth could eventually require surgery or extraction.
Some infections progress quietly with no pain at all, which makes a timely evaluation even more valuable. A thorough checkup can surface hidden problems before they become emergencies.
Warning Signs Your Tooth May Need Endodontic Care
Your tooth has specific ways of signaling distress. Pain, temperature sensitivity, and gum changes are the most telling early signs that the inner structures may be compromised.
When Tooth Pain Lasts Longer Than It Should
A dull ache that lingers for hours, or sharp pain when you bite down, isn't something to wait out. The discomfort may stay in one spot or spread to your jaw, face, or neighboring teeth.
Pay close attention if pain wakes you at night or gets worse when you lie down. That pattern points to inflammation or infection inside the tooth, and ignoring it almost always leads to a more serious situation.
What Prolonged Temperature Sensitivity Really Means
A quick twinge from cold water is normal. What isn't normal is when that sensitivity hangs around for 30 seconds or more after the hot or cold source is gone.
You might feel it with coffee, ice cream, or cold air, like a sharp sensation that makes you stop mid-sip. When the pain lingers, intensifies over time, or pushes you to avoid certain foods, it's a sign the nerve inside the tooth is exposed or damaged.
What Gum Swelling and Tenderness Are Telling You
Swelling near a tooth usually appears as a puffy, tender patch on the gum. Sometimes a small raised bump develops that looks like a pimple. The area may feel warmer than the surrounding tissue, or you might notice an unpleasant taste.
If the swelling doesn't clear up within a day or two — or keeps coming back in the same spot — it won't resolve on its own. Swelling that spreads to your face or jaw is a reason to call your dentist promptly.
Subtle Symptoms That Are Easy to Miss
Not every endodontic problem is obvious. A color change, a recurring bump, or unexplained jaw discomfort can all point to something deeper that's easy to overlook.
A Single Darkening Tooth
When one tooth starts turning gray, dark yellow, or brown, it often means the pulp inside is dying. As the internal tissue breaks down, pigment leaches inward and stains the tooth from the inside out.
Because this process is frequently painless, it's easy to ignore. But a darkening tooth still needs evaluation, even when it's completely comfortable. Common causes include old trauma, deep decay, prior dental work that has failed, or natural aging of the pulp tissue.
Recurring Bumps on Your Gums
Small pimple-like bumps on your gums are typically dental abscesses or fistulas: pockets of infection that find an escape route through the gum tissue. They may drain, temporarily disappear, and then return to the exact same spot.
That cycle of coming and going is the warning sign. The bump might not hurt much, which is exactly why people tend to ignore it. But a painless bump still signals an active infection that needs treatment.
Jaw Pain
Jaw pain that worsens when you chew can actually originate from a tooth, not the jaw joint itself. Infected tooth roots send pain signals to the surrounding tissue, mimicking a muscular ache or a TMJ issue.
You might find yourself unconsciously shifting to chew on the other side, or notice one tooth feels slightly higher than the rest. Both are signs that inflammation is building around the root tip, and are worth mentioning to your dentist.
What Puts You at Higher Risk for Endodontic Problems
Some people are significantly more likely to need endodontic care based on their dental history. Knowing your risk factors helps you and your dentist monitor the right teeth before symptoms develop.
How Past Tooth Injuries Increase Your Risk
Any blow to your teeth raises your risk, even if the tooth looked fine immediately after. The blood supply inside can become compromised without producing immediate pain, and damage to the pulp may not surface for weeks, months, or years.
After any dental trauma, keep an eye out for discoloration, temperature sensitivity, pain when biting, or gum swelling near the affected tooth. Always let your dentist know about past injuries so they can track changes over time.
Why Deep Decay Often Leads to Endodontic Treatment
Cavities that reach close to or into the pulp create a direct pathway for bacteria to infect the tooth's inner tissue. Deep decay usually starts small and advances slowly, sometimes with no pain at all until it's already serious.
When a cavity is too deep for a filling, endodontic treatment may be the only way to save the tooth. Regular checkups catch decay while it's still shallow, when your options are simpler and less invasive.
How a Tooth's Dental History Affects Its Long-Term Health
Teeth that have had multiple fillings, crowns, or other restorations are more vulnerable to pulp problems over time. Each procedure reduces the remaining tooth structure and places cumulative stress on the nerve tissue inside.
If a particular tooth has an extensive history, any new symptom it develops deserves close attention. What feels like a minor change in comfort could be an early signal that the pulp is beginning to fail.
How to Prepare for Your Endodontic Evaluation
Recognizing the warning signs is the first step. Acting on them promptly is what protects your tooth. Here's what to do next.
When to Call Your Dentist About Tooth Pain
Call your dentist if tooth pain lasts more than a day or two, especially if it wakes you at night or gets worse when lying down. Gum or facial swelling, lingering temperature sensitivity, or a recurring bump on your gum are all reasons to schedule a visit sooner rather than later.
Your dentist will examine the tooth, likely take X-rays, and decide whether to treat it in-office or refer you to an endodontist.
Questions Worth Asking Before Your Treatment Begins
Before treatment starts, ask your specialist to walk you through what the procedure involves and why it's the right approach. Knowing the plan reduces anxiety and helps you make a confident, informed decision.
Other questions worth raising:
Will I need a crown or other restoration afterward?
What are the costs, and is this covered by my insurance?
What are the risks of leaving this untreated?
How long should the treated tooth last?
How to Get Ready for Your First Endodontic Appointment
Bring your insurance card and a valid ID so coverage can be verified without delays. If your general dentist hasn't forwarded recent X-rays, bring any images from the past six months, as they give the endodontist a valuable starting point. Write down every medication, vitamin, and supplement you take, since some can affect treatment or healing.
Jot down your symptoms before you go: when the pain started, what makes it better or worse, and whether it's constant or comes and goes. That detail helps your specialist assess your situation faster. Eat beforehand, since you may have some numbness after treatment, and avoid alcohol for 24 hours prior to your appointment.
Your Smile Is Worth Protecting. Don't Wait For The Warning Signs
Tooth pain, swelling, or sensitivity that keeps coming back aren't problems that resolve on their own. Catching them early gives you more options, simpler treatment, and a much better outcome for your long-term oral health.
At See Me Smile Dental & Orthodontics, we make it easy to get answers without the runaround. Our team handles both dental and endodontic care under one roof, with flexible scheduling and financing options to keep treatment accessible.
If something feels off, trust that instinct. Call our Santa Barbara office or schedule your visit online —we're here to help you figure out exactly what's going on and what to do next.
How do I know if my tooth pain is serious enough to see an endodontist?
Pain that lasts more than a day or two, wakes you at night, or gets worse when you lie down is worth a prompt call to your dentist. Lingering temperature sensitivity, gum swelling, or a recurring bump near a tooth are also signs that something deeper may be going on. When in doubt, schedule a visit — catching a problem early almost always means simpler treatment.
What does a root canal actually feel like?
Most patients are surprised by how comfortable the procedure is. Modern techniques and local anesthesia keep discomfort minimal during treatment, and any soreness afterward typically fades within a few days. For most people, the anxiety leading up to it is far worse than the procedure itself.
Can a tooth need endodontic treatment even if it doesn't hurt?
Yes. Some infections and pulp problems develop slowly and quietly, with no pain at all. Tooth discoloration, a recurring bump on the gum, or a tooth that feels slightly different when you bite can all point to an underlying issue — even when there's no discomfort. This is one of the strongest reasons to keep up with regular dental checkups.
How long does a root canal procedure take?
Most root canals are completed in one or two appointments, each lasting between 60 and 90 minutes, depending on the complexity of the case. Your dentist or endodontist will give you a clearer timeline once they've assessed your tooth and confirmed the treatment plan.
What happens if I delay endodontic treatment?
An untreated infection doesn't stay contained — it can spread to surrounding teeth, your jawbone, or other areas of your body. What might have required a straightforward root canal can progress to the point where surgery or extraction becomes the only option. Acting promptly protects both your tooth and your overall health.
Is it possible to need a root canal after a tooth has already been treated?
Yes. A previous root canal can occasionally fail to heal as expected, or new decay can create a fresh pathway for bacteria to re-enter the tooth. In these cases, retreatment — redoing the root canal — is often a highly effective option for saving the tooth.
How soon can I return to normal activities after a root canal?
Most people return to work or their regular routine the same day or the day after treatment. You may notice some mild soreness when biting for a few days, which over-the-counter pain relief typically manages well. Your dentist will walk you through any specific aftercare steps before you leave the office.


![Best Ways to Protect a Chipped Tooth Before Treatment [Essential Guide]](https://dropinblog.net/cdn-cgi/image/fit=scale-down,format=auto,width=700/34264081/files/featured/chipped-tooth-protection-before-treatment-santa-barbara.png)